chronic mucocutaneous candidiasis
Diseases of the nails can cause significant social, psychological, and physical damage to an affected individual. These disorders may be isolated to the nail unit itself or be part of a larger systemic disease that may present first, or only, in the nail unit. The image shown is of an individual with chronic mucocutaneous candidiasis.

The nail unit is composed of the nail plate, the nailbed, the hyponychium, the nail matrix, the nail folds, the cuticle, the anchoring portion of the nailbed, and the distal phalangeal bones. The nail plate is the largest component of the nail unit. The nail matrix gives rise to the nail plate. Any defect to the matrix results in onychodystrophy of the growing nail plate. The proximal nail matrix forms the dorsal portion of the nail plate, whereas the distal matrix forms the ventral part of the nail plate. Clinical disease may vary depending on the location and the severity of inflammation of the affected nail unit.
Onychomycosis
Onychomycosis is a fungal infection involving any component of the nail unit. It may cause pain, discomfort, and disfigurement that can lead to physical and occupational limitations. Trichophyton rubrum and T mentagrophytes are responsible for 90% of all cases of onychomycosis. Most commonly the fungus spreads from the plantar skin and invades the nailbed via the hyponychium. Onychomycosis is typically asymptomatic. Patients tend to request help for cosmetic reasons but occasionally complain of pain, discomfort, and loss of dexterity. Treatment involves topical or oral antifungals depending on the location and extent of infection.
Clubbing
Clubbing is a clinical finding characterized by bulbous fusiform enlargement of the distal portion of a digit in which the angle between the proximal nail fold and the nail plate decreases to less than 160°. The exact pathophysiologic mechanism is unknown. Primary clubbing is caused by pachydermoperiostosis, familial clubbing, and hypertrophic osteoarthropathy. Causes of secondary clubbing include disorders of the lungs (such as lung cancer, interstitial lung disease, cystic fibrosis), heart (including cyanotic congenital heart disease), gastrointestinal tract (such as inflammatory bowel disease, liver cirrhosis, achalasia), and skin (as exemplified by palmoplantar keratoderma), as well as many malignancies, such as thyroid cancer, chronic myeloid leukemia, and other miscellaneous conditions, including acromegaly and pregnancy. There is no specific treatment for clubbing. If the underlying disease process or condition is treated, then the clubbing may improve or resolve.
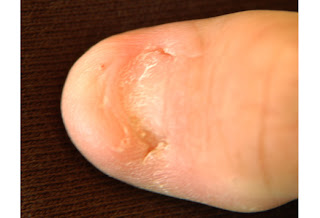
Paronychia
Paronychia is a soft-tissue infection of the crease between the nail and the nail fold (shown). It is the most commonly encountered hand infection, often seen in individuals whose occupation requires frequent contact with water, such as bartenders. Patients typically describe pain and tenderness. Acute paronychia typically develops after minor trauma and can lead to infection, with Staphylococcus aureus as the organism most commonly implicated in infection. Chronic paronychia develops after exposure to moist environments and lasts 6 weeks or longer, with Candida albicans as the most common etiologic agent. On examination, the affected area may appear erythematous and swollen with pus in advanced cases and nail changes in chronic ones. Acute paronychia is treated with warm soaks and oral antibiotics. Chronic paronychia is treated by keeping the lesion dry and by the application of topical antifungals. Surgical intervention may be required in acute or chronic paronychia cases that are refractory to therapy or in which an abscess develops.
Melanonychia
Melanonychia is a brown or black pigmentation of the nail plate. It most often occurs because of increased production of melanin by melanocytes in the nail matrix. It is more common in darkly pigmented individuals and may be found in almost 100% of African Americans over the age of 50 years. There are 2 types of melanonychia: diffuse and longitudinal. Distinction depends upon the extent of discoloration. It may be caused by a number of different conditions, including melanocytic hyperplasia in melanoma (shown), lentigo, melanocytic nevi, physiologic causes (including darker skin tone and pregnancy), local factors (such as trauma, carpal tunnel, and ultraviolet light), systemic diseases (including hyperthyroidism, Addison's disease, systemic lupus erythematosus, and vitamin B12 deficiency), and dermatologic disorders (such as psoriasis vulgaris, progressive systemic sclerosis, and lupus erythematosus), or iatrogenically by medication, especially chemotherapeutic agents and antibiotics. Patients are typically asymptomatic; treatment is aimed at correction of the underlying process.
Distal onycholysis
Distal onycholysis refers to spontaneous separation of the nail plate starting at the distal free margin and progressing proximally. Local irritation is the most common insult, such as excessive filing or chemical overexposure in manicures. Onycholysis has also been associated with a number of other systemic disorders, specifically systemic lupus erythematosus, hyperthyroidism, iron-deficiency anemia, primary dermatologic diseases (such as atopic dermatitis and psoriasis vulgaris), or neoplasms (including squamous cell carcinoma and lung carcinoma), as well as medications (especially fluoroquinolones and doxycycline), infections, or congenital etiologies. Patients do not typically report any pain or discomfort unless there is a superimposed infection. Treatment involves controlling or eliminating any risk factors and clipping off the unattached nail to prevent additional prying off and to allow for normal replacement of nail growth.
Subungual hematomas
Subungual hematomas are common nailbed injuries caused by blunt or sharp trauma to the nail. The rich vascular supply in the nailbed makes it prone to bleeding. Patients with minor hematomas are typically asymptomatic. Large hematomas may produce enough throbbing pain for patients to seek medical attention. Treatment involves trephination, in which a hole is drilled or burned through the nail body to release pressure, or nail removal.
Onychocryptosis
Onychocryptosis refers to an ingrown toenail, typically found in the big toe. Extrinsic compression of a toenail, typically from tight footwear, places constant pressure on the nail wall. If the nail is cut inappropriately short and the nail fold is irritated or penetrated, then colonization of bacteria or fungi may occur. Inflammation, edema, erythema, and pain are common findings; an abscess or cellulitis may develop. Treatment for early inflammation focuses on avoiding compressive footwear, dislodging the embedded nail plate, and education on proper nail care, including trimming the nail with squared corners. Treatment for more advanced cases involves partial or complete toenail removal. Antibiotic therapy is typically not required except for those who are diabetic, immunocompromised, or who show significant evidence of cellulitis.
Nail-patella syndrome
Nail-patella syndrome is an autosomal dominant condition characterized by nail dysplasia (shown), patellar aplasia-hypoplasia, elbow arthrodysplasia, and iliac horns. The nails may be absent, hypoplastic, or dystrophic with ridges, pits, and/or triangular lunulae. The anomalies are typically symmetric with the thumbs most severely affected and decreased severity progressing towards the fifth digit. Anomalies are evident at birth. Patients may also suffer from proteinuria, glaucoma, attention-deficit/hyperactivity disorder, recurrent dislocations, and irritable bowel syndrome. Treatment is aimed at pain management, physical therapy, and controlling renal failure. No specific therapy is available for the nail anomalies.
Psoriatic nail disease
Psoriatic nail disease is deformation of the nail unit of unclear etiology. It typically occurs in patients with clinically evident psoriasis and rarely is the only cutaneous finding. The clinical manifestations are protean and depend upon the portion of the nail unit affected. Findings may include pitting, Beau's lines (transverse lines in the nail caused by intermittent growth arrest), salmon patches, subungual hyperkeratosis, onycholysis, nail plate crumbling, splinter hemorrhages, and a spotted lunula. Diagnosis is made on clinical findings or by a nail biopsy. Treatment focuses on the functional and psychosocial aspects of the disease, as no curative treatment is available. Options include corticosteroids, psoralen plus ultraviolet light (PUVA), chemotherapeutic agents, and avulsion therapy.









Dry cracked feet are never attractive or comfortable. Aging and normal activity cause the padding to deteriorate on the soles of your feet. The feet become more tender and prone to dryness and injury. Calluses, dry heels, and thickened cuticles form.Nailexpert by Wartner
BalasHapus